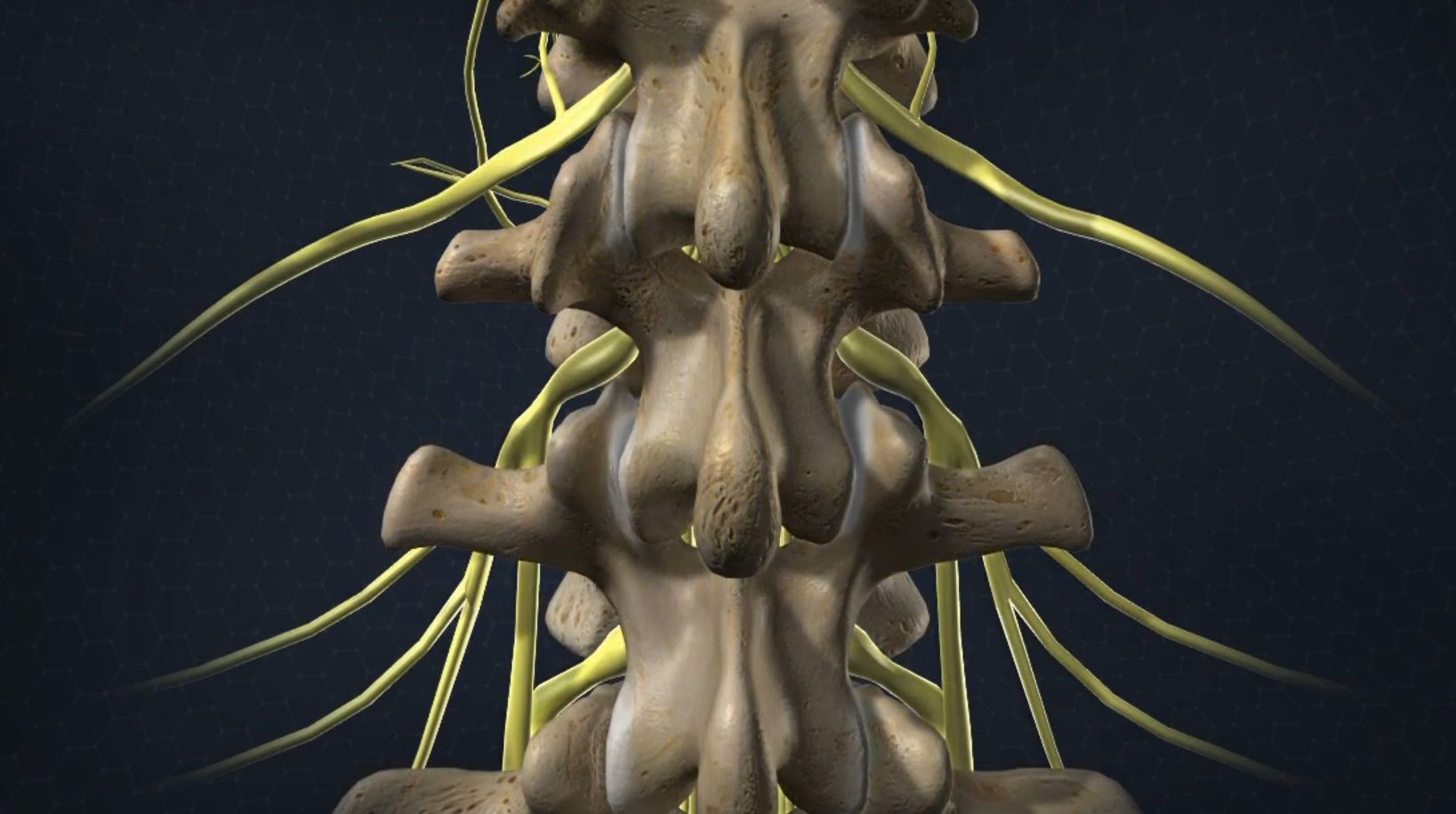
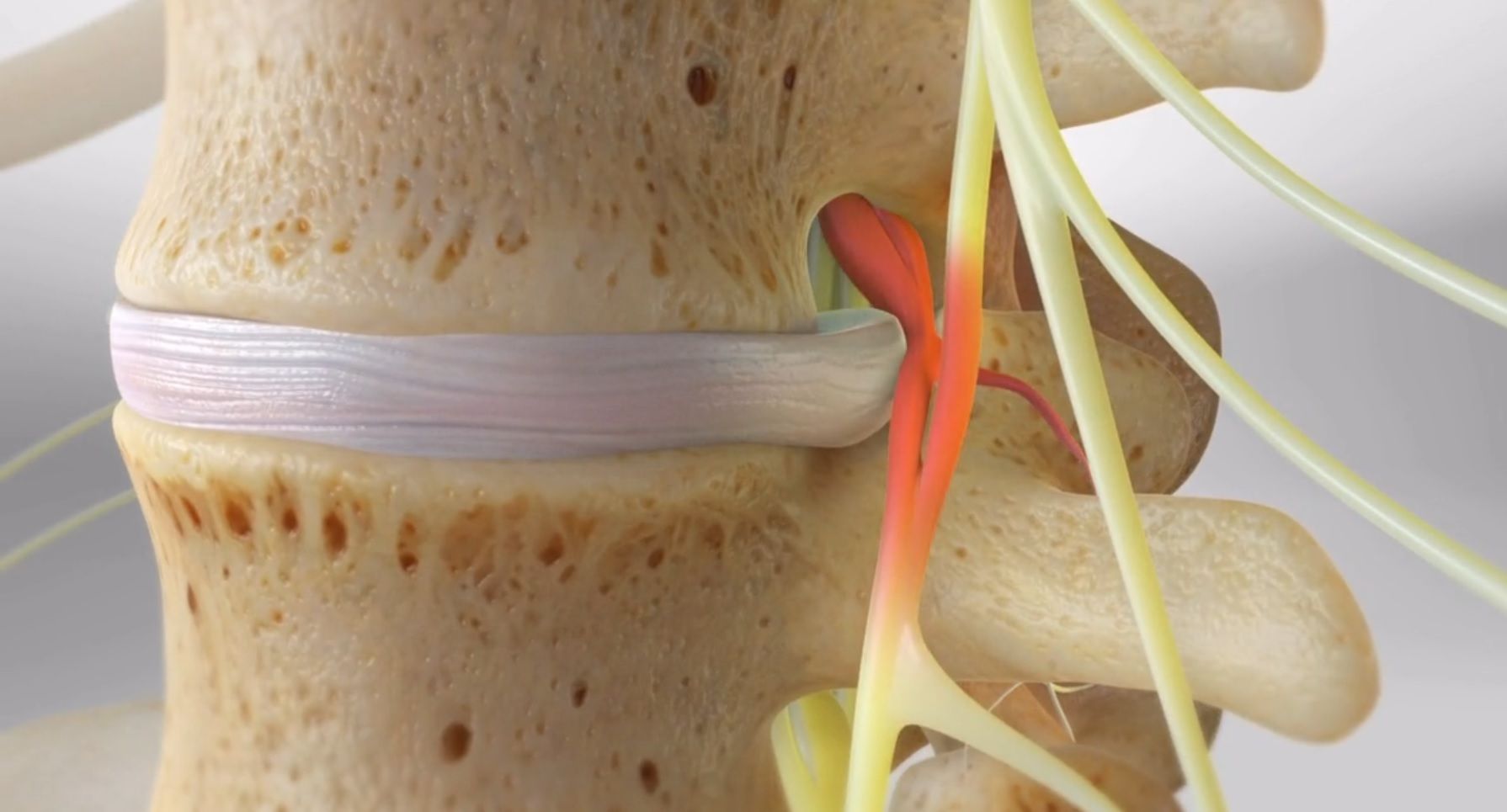
Lumbar Discoscopic Discectomy
This minimally-invasive procedure is designed to relieve pain caused by herniated discs pressing on nerve roots. This surgery is performed through a small tubular device under local or epidural anesthesia, allowing the patient to leave the hospital the same day.
Lumbar Discoscopic Discectomy
Lumbar Discoscopic Discectomy
Overview
A Lumbar Discoscopic Discectomy is a minimally-invasive, outpatient surgery that relieves nerve pain caused by herniated discs. It is performed through a small tubular device under local anesthesia.
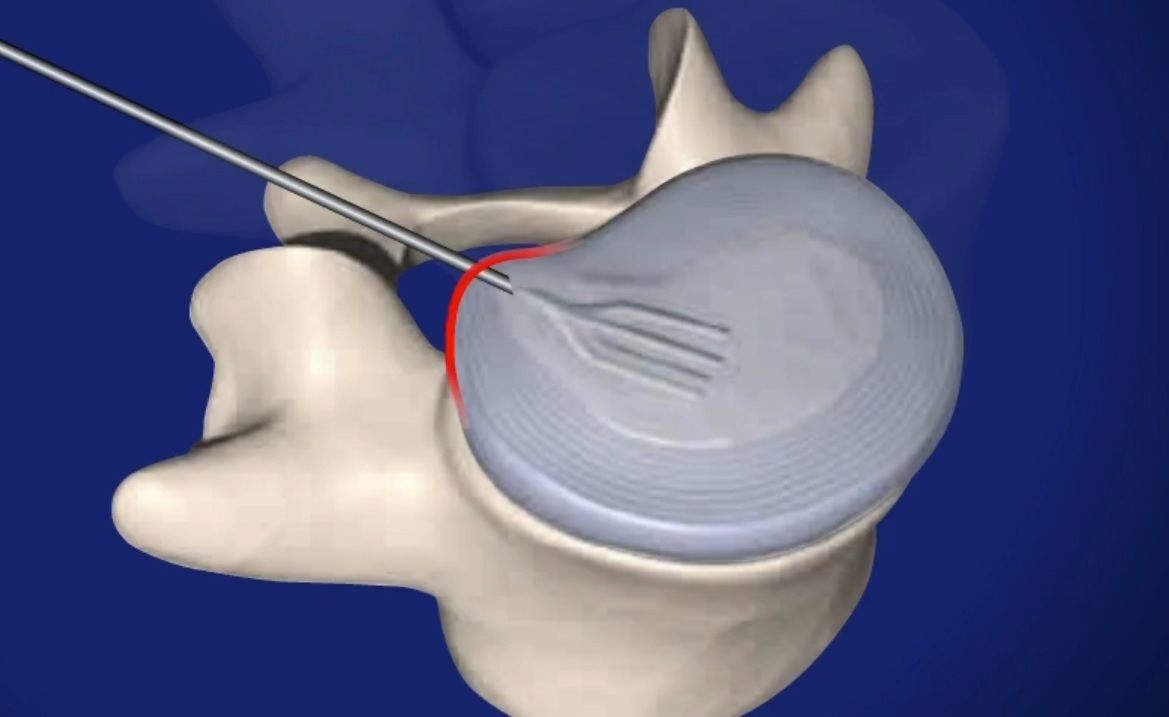
Guide Wire Inserted
The surgeon uses a fluoroscope (video x-ray machine) to find the correct route to the injured disc. The surgeon then inserts a guide wire into the disc.
Dilating Tube Inserted
A dilating tube is slid over the guide wire, pushing tissue and nerve roots aside. Additional anesthesia is used to numb painful tissue along the path.
Working Sleeve Positioned
The surgery will be performed through a single working sleeve. This is slid over the dilating tube down to the herniated disc. The surgeon then removes the guide wire and dilating tube.
Endoscope Inserted
The surgeon uses an endoscope containing a light and a small camera. A video monitor displays the camera’s view. This allows the surgeon to visualize the herniation, guide the surgical tools, perform the procedure, and inspect the results.
Disc Portions Removed
The surgeon uses surgical instruments to remove the parts of the disc pressing on the spinal nerves.
Disc Wall Treated
To keep the disc contents inside the disc, the damaged disc wall is treated with a laser or a radiofrequency probe (RFA). The surgeon inspects the vertebra and nerves to confirm successful decompression.
End of Procedure
The instruments, endocope, and working sleeve are removed. The insertion area is bandaged. Recovery is quick and with minimal scarring. The patient is sent home that same day and is usually able to return to normal activities within a few weeks.
Revised from www.viewmedica.com © Swarm Interactive. Unauthorized duplication is strictly forbidden.
- Category / Surgery